Abstract
Background: Avatrombopag (AVA) is an oral, thrombopoietin receptor agonist approved by FDA for the treatment of thrombocytopenia in patients with chronic liver disease scheduled to undergo a procedure. AVA is also being developed for other indications including chronic immune thrombocytopenia (cITP) (Bussel et al, Blood, 2014; Wojciech et al, Br J Haematol, in press 2018). In repeated-dose studies in mice, rats and cynomolgus monkeys, there were AVA dose, concentration, and duration-dependent histologic changes in gastric fundic glands that reversed by 4 weeks after dosing was stopped. This was associated with decreased gastric acid production, hypergastrinemia, and increased intragastric pH in all species. The NOAEL in 2-year toxicology studies was defined at exposures 4 to 21-fold the recommended human AVA dose.
Hypergastrinemia and parietal cell hyperplasia have also been reported with proton pump inhibitors (PPIs) and H2-receptor antagonists (H2RA). These findings may be secondary to suppression of gastric acid production, and, in rodents, may lead to gastric carcinoids. Findings of hypergastrinemia-related gastric hyperplasia in rodents have a low risk/relevance to humans.
To further evaluate the preclinical findings and screen for atrophic gastritis, gastric biomarkers (gastrin, gastrin-17, and pepsinogen I/II [PG-I/PG-II]) were measured in 2 Phase 3 trials with chronic AVA dosing. These multicenter, randomized, controlled Phase 3 trials were conducted in patients with cITP, and assessed clinical safety and efficacy of AVA versus placebo (PBO) (Study 1- NCT01438840) or eltrombopag (ELT) (Study 2- NCT01433978); Study 2 was terminated early due to enrollment challenges.
Methods: Both Phase 3 trials enrolled adults (≥18 years) with chronic ITP (Baseline platelet count (PC) <30x109/L), who were randomized 2:1 to receive either 20 mg/day AVA or PBO (Study 1) or 1:1 to 20 mg/day AVA or ELT (50 mg/day) (Study 2) orally with food for 26 weeks. Individual patient AVA (5-40 mg/day) or ELT (25-75 mg/day) dose titration was permitted.
Patients with Baseline fasting gastrin-17 levels greater than upper limit of normal (ULN) were excluded from the study, as were patients taking PPIs or H2RAs if not on a stable dose or if gastrin-17 levels were >1.5 times the ULN.
Safety analyses included adverse event (AE) monitoring and laboratory testing, including fasting gastric biomarkers. Patients who developed 2 consecutive fasting gastrin-17 levels >2.5 times the ULN or low serum PG-I levels or low PG-I/PG-II ratio (with low fasting gastrin-17 levels) were to be discontinued from the trials. Patients with elevations >5 times the ULN were to undergo endoscopy to assess the gastric mucosa.
Results: A total of 64 patients were treated with AVA across the two trials (Study 1 n=47; Study 2 n=17); the majority were white (92.2%) and female (64.1%), with a mean age of 46.6 years. The median duration of exposure to AVA was 35.1 weeks, with a mean daily dose of 24.6 mg; 75% of subjects received AVA doses between 5 and 40 mg for ≥20 weeks. AVA was shown to be superior to PBO in the median cumulative number of weeks of platelet response (PC ≥50×109/L in the absence of rescue therapy) in Study 1 (12.4 vs. 0.0 weeks, respectively; p <0.0001). Mean Baseline PCs in Study 1 were similar in AVA- and PBO-treated subjects (14.1 and 12.7x109/L, respectively), and peaked at 205.4 and 11.6x109/L on Week 2; mean Baseline PCs were lower in Study 2 in AVA- compared to ELT-treated subjects (13.0 and 18.2x109/L, respectively), and increased to 184.8 and 91.6x109/L at Week 2.
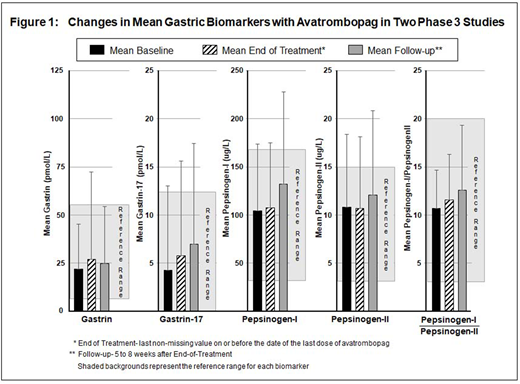
Of the AVA-treated patients, no significant changes in the mean fasting gastrin, gastrin-17, PG-I, PG-II, or the PG-I/PG-II ratio were observed from Baseline over the course of the trial (Figure 1). In addition, no patients met the gastric biomarker change criteria for discontinuation or to undergo endoscopy. Common AEs in Study 1 included headache, contusion and upper respiratory tract infections, with 4 cases of thromboembolic events.
Conclusions: In Phase 3 trials, AVA was shown to be effective and well tolerated in the treatment of thrombocytopenia in patients with cITP, with most patients demonstrating substantial platelet increases. In particular, treatment of cITP with AVA was not associated with an increase in gastric biomarkers including gastrin, gastrin-17 or pepsinogen and, therefore, no signal of gastric toxicity was identified with chronic AVA dosing of up to 26 weeks.
Bussel:Prophylix: Consultancy, Research Funding; Protalex: Consultancy; Amgen Inc.: Consultancy, Research Funding; Uptodate: Honoraria; Rigel: Consultancy, Research Funding; Momenta: Consultancy; Novartis: Consultancy, Research Funding. Allen:Dova Pharmaceuticals: Employment, Equity Ownership. Tian:Dova Pharmaceuticals: Employment, Equity Ownership. Kuter:Pfizer: Consultancy; ONO: Consultancy; Amgen Inc.: Consultancy; Novartis: Consultancy; Syntimmune: Consultancy; Protalex: Research Funding; Rigel: Consultancy, Research Funding; Argenx: Consultancy; Dova Pharmaceuticals: Consultancy, Membership on an entity's Board of Directors or advisory committees; Bioverativ: Consultancy, Research Funding; BMS: Research Funding; Principia: Research Funding.
Author notes
Asterisk with author names denotes non-ASH members.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal